By David Blyweiss, M.D., Advanced Natural Wellness
November 6, 2020
I’m having a pizza this weekend!
It’s been a few months. Mmm… I’m going to have a thin crust, crispy, Hawaiian pizza. People think I’m crazy, but I think it’s the best kind.
There’s just something about that pineapple sweetness along with the Canadian bacon taste. It’s the perfect treat.
Normally, a slice of pizza is not a part of my regular diet. Instead, I focus on mostly plant-based rainbow foods. This helps keep my gut microbiome healthy so my entire body and mind is working at top level.
There’s another reason I eat the way I do. It has to do with the health of my gut lining.
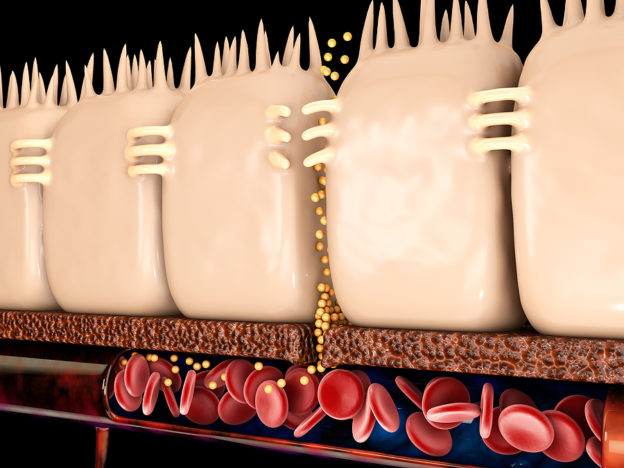
When you really think about it, the contents of your gut and your intestine only have about one cell separating them from the rest of your body. Within that cell membrane, there are tight junctions that keep nasty things like bacteria or large food particles from leaking out into your body.
But when you open up that door – with something commonly called a “leaky gut” – you’re leaving your body vulnerable to bacteria, viruses and macromolecules of food particles entering the bloodstream.
Open your arteries, improve blood flow for a new health miracle...
Did you know your circulatory system has over 60,000 miles of arteries, veins and other blood vessels, if stretched end to end?
But as you age, your blood vessels undergo changes, which may cause them to stiffen, thicken and get clogged.
GOOD NEWS! Doctors have now identified a “Miracle Molecule” inside your arteries that helps OPEN your arteries and IMPROVE blood flow.
It’s what Dr. Valentin Fuster calls it, "One of the most important discoveries in the history of cardiovascular medicine."To you, that means...
- Healthy blood pressure
- Sharper mind and memory
- Skyrocketing energy and muscular strength
- Increased pleasure and passion in the bedroom
- Improved circulation to every cell and organ in your body
Go here to discover a new natural way to significantly boost the levels of this miracle molecule in YOUR body NOW!
Gluten is Like an Addictive Drug
Sometimes, foods that don’t fully digest, like gluten (a protein found in wheat), also leak out.[1] This new, partially digested and transformed protein is called gluteomorphin and with it’s attendant breakdown product of gliadomorphin component also gaining access to your bloodstream… your body reacts.
People who react to gluten are said to have celiac disease, wheat allergy, or non-celiac gluten sensitivity (NCGS). NCGS shows symptoms like abdominal pain, bloating, diarrhea, constipation, “foggy mind,” headache, fatigue, joint, and muscle pain.[2] In short, it’s no fun.
Pay close attention to those word – gluteomorphin and gliadomorphin. The second half of it holds the key here. Just like morphine, gluten is indeed addictive. It goes through your blood-brain barrier and makes you want to eat more and more gluten.
This is bad news for your body. Harvard medicine found that it only takes a thumb-sized amount of gluten to cause the gut to become leaky.[3]
Understanding how gluten affects the body is a big reason why we see so many more “gluten-free” foods these days. About 41% of foods are available in a gluten-free version at the store.[4] (Your grocery bill won’t appreciate these purchases though. They can be pricey.)
How to Escape the Leaky Gut Cycle
Once your gut begins to leak, you will become ill, but it could be at such a low level that you don’t even realize you’re sick. You’ll think you’re just a little bit fatigued or a smidge tired. Maybe you’re not thinking as clearly.
You start to think, “Oh, I’ll have that pizza tonight.” Or, “Instead of a salad, I’ll have a sandwich today.” Or, “I need pasta, now!”
These little voices are your bad gut bacteria telling you to have gluten or other problem foods because you’ve become addicted. Bad bacteria will crave more bad foods. On the flip side, good bacteria in your gut will crave more healthy fruits and vegetables.
Are You Suffering From...
- Love handles and a pot belly
- Romance that isn't what it used to
- Forgetfulness and inattention
- Low (or no) strength and endurance
- A sex drive that's shifted into neutral...or worse
If so...you may have Mature Male Burnout. Click here to discover more about this unique condition and what you can do about it.
These healthy foods allow you to make enough butyrate, a fatty acid that helps heal the lining of your colon.[5]
Really, it’s a big cycle… eat bad foods and become addicted to more bad foods. Or, break the cycle and eat health foods, crave more healthy foods, and produce an acid that actually heals your gut.
It’s your decision to make.
Besides foods, there are some other causes of leaky gut – also known as abnormally increased intestinal permeability.
Intestinal permeability is increased in patients with Crohn’s disease. It’s also higher in people with celiac disease and in those who have suffered from trauma, burns and too many NSAID medications.[6]
Since there is a gut-brain connection, any trauma to the brain will send signals down your vagus nerve to the gut.[7] Within just a few hours, your gut will start feeling the negative effects.
Acute stress can also cause a leaky gut and make you feel ill. This explains why your stomach feels like it’s doing flip-flops before you walk on stage to address a large crowd.
Then, stress disorders like endurance exercise, pregnancy, and certain foods can increase permeability.[8]
Drugs like non-steroidal anti-inflammatories (NSAID) pain relievers can cause a leaky gut. Anyone who is dealing with chronic stress headaches or certain body aches and pains may be popping two or three Advil (ibuprofen) two or three times a day.
This means they are also ruining their gut lining each time they take a dose. They are also potentially ruining their kidney function. Nearly 16,500 people die each year from taking NSAIDs.[9]
If you want to avoid leaky gut, here’s what I recommend:
First off, eat the right foods. Remember, healthy vegetables and fruits from every color in the rainbow will promote a health gut microbiome which is good for your gut lining. Then, I like to drink kombucha every night or enjoy other fermented foods like kimchi to promote a healthy gut.
Practice mindful breathing each day to decrease stress levels. Lastly, I have a machine called a Healy machine[10] that changes the resonance in my body, of every cell, to bring them back to optimal functioning. It’s a bit expensive, but I do whatever I can and it makes me feel a lot better.
Sources:
[1] Wieser, Herbert. “Chemistry of gluten proteins.” Food microbiology 24.2 (2007): 115-119.
[2] Catassi, Carlo. “Gluten sensitivity.” Annals of nutrition and metabolism 67.Suppl. 2 (2015): 15-26.
[3] Putting a stop to leaky gut. Harvard Health Publishing, Harvard Medical School, Dec 2018. Available Online: https://www.health.harvard.edu/diseases-and-conditions/putting-a-stop-to-leaky-gut
[4] Singh, J., and K. Whelan. “Limited availability and higher cost of gluten‐free foods.” Journal of Human Nutrition and Dietetics 24.5 (2011): 479-486.
[5] Hamer, Henrike M., et al. “The role of butyrate on colonic function.” Alimentary pharmacology & therapeutics 27.2 (2008): 104-119.
[6] Hollander, Daniel. “Intestinal permeability, leaky gut, and intestinal disorders.” Current gastroenterology reports 1.5 (1999): 410-416.
[7] Fülling, Christine, Timothy G. Dinan, and John F. Cryan. “Gut microbe to brain signaling: what happens in vagus….” Neuron 101.6 (2019): 998-1002.
[8] Camilleri, Michael. “Leaky gut: mechanisms, measurement and clinical implications in humans.” Gut 68.8 (2019): 1516-1526.
[9] Graham, David Y., et al. “Visible small-intestinal mucosal injury in chronic NSAID users.” Clinical Gastroenterology and Hepatology 3.1 (2005): 55-59.
[10] Healy. Available Online: https://www2.healy.shop/en-us/