By David Blyweiss, M.D., Advanced Natural Wellness
December 13, 2021
During the past two years during the COVID pandemic, a lot of people have put off their regular doctor’s visits. But delaying or avoiding healthcare is never a good idea, even if you have no known health conditions.
There are a lot of health issues that can sneak up on you, and are often only discovered when you get your annual checkup.
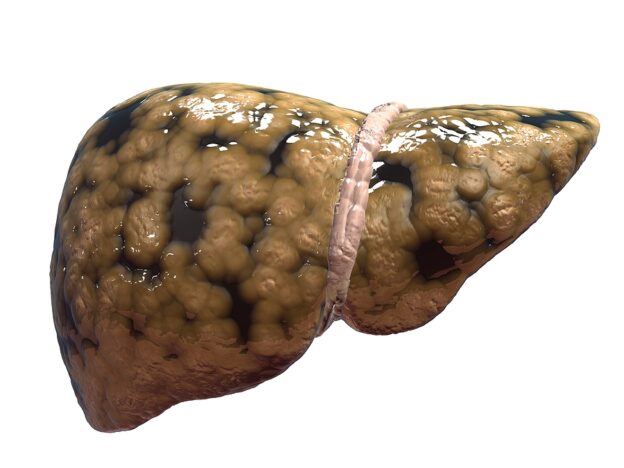
One that I find very concerning is non-alcoholic fatty liver disease, or NAFLD. There aren’t any symptoms ahead of time. So people are walking around with the beginnings of a very serious liver disease, and they don’t even know it. But if it’s not diagnosed and treated early, it can become very aggressive. It can even advance to cirrhosis and liver failure.
Here in the U.S. it’s the most common form of chronic liver disease. It affects somewhere between 25% and 30% of all U.S. adults. But it didn’t used to be that way.
We didn’t have any appreciable levels of non-alcoholic fatty liver disease before corn syrup and high fructose corn syrup came on the market. And we didn’t have NAFLD as the number two reason for liver transplants in the U.S…. or in people in their 20’s, 30’s and 40’s.
In fact, NAFLD was so uncommon that it wasn’t even given a name until 1980. Coincidentally, high fructose corn syrup was introduced to the food and beverage industry in the 1970s.
Open your arteries, improve blood flow for a new health miracle...
Did you know your circulatory system has over 60,000 miles of arteries, veins and other blood vessels, if stretched end to end?
But as you age, your blood vessels undergo changes, which may cause them to stiffen, thicken and get clogged.
GOOD NEWS! Doctors have now identified a “Miracle Molecule” inside your arteries that helps OPEN your arteries and IMPROVE blood flow.
It’s what Dr. Valentin Fuster calls it, "One of the most important discoveries in the history of cardiovascular medicine."To you, that means...
- Healthy blood pressure
- Sharper mind and memory
- Skyrocketing energy and muscular strength
- Increased pleasure and passion in the bedroom
- Improved circulation to every cell and organ in your body
Go here to discover a new natural way to significantly boost the levels of this miracle molecule in YOUR body NOW!
Seriously, it’s the high fructose corn syrup that’s ruining your liver.
The thing is, many people don’t really count HFCS as sugar, because it’s hidden in most processed foods. But the fructose in the corn syrup doesn’t get metabolized the way that glucose sugar does. It just hangs on to your liver and causes all of these problems.
Also, I know people who use agave syrup instead of sugar. Well look at the label. Agave is one of the highest fructose sweeteners on the market… even worse than HFCS. So you hear that agave is healthier. Well, no. Not for you’re liver. It’s basically fructose.
So please! Read labels. High fructose corn syrup is hidden is so many things, even ones that you don’t perceive as sweet.
Acetaminophen – The Most Dangerous Drug for Your Liver
And acetaminophen? It’s just horrible for your liver. It irreversibly reduces glutathione that your liver needs to make to protect you.
Interestingly, acetaminophen wasn’t available in Europe until about 20 years after it came out here in the U.S. So people visiting here from overseas would take Tylenol® back with them for hangovers. And, unfortunately, the Europeans drink, whether they’re Irish or Scottish or English or French or Italian. They drink a lot.
The World's Quickest Solution for Ending Prostate and Urinary Misery
This has recently been revealed to be one of the only real breakthroughs in prostate health.
The seeds of a strange fruit (sometimes called "Chinese Apples") hold powerful phytonutrients that are a revolution in prostate health.
In fact, UCLA and Veterans Administration research have now proved this to be true.
Not only that, but it may be the worlds quickest solution for ending prostate misery.
Simply stated, these phytonutrients represent a huge step beyond beta sitosterol, saw palmetto, and other phytosterols alone.
Simply click HERE if you want to have fast prostate relief...restful, uninterrupted sleep...no more constant "urges to go"...enhanced virility...and optimal prostate support for life.
Well, they wound up having all of these liver comas and ending up in the ER. The worst thing you can do is mix Tylenol® and alcohol.
And then there were people trying to protect themselves from getting a migraine. They were taking two or three or four Tylenol® before going to bed. And they weren’t waking up.
So it’s not surprising that acetaminophen contributes to over half of all liver failure cases in the U.S. It’s probably one of the most dangerous drugs in medical use, and it’s sold over-the-counter. Yet accidental overdose of acetaminophen has been a problem for decades.
And by the way. If you think you’re safe because you’re using it “properly,” think again. Tylenol PM is a perfect example.
This is a combination of acetaminophen and Benadryl®. People take if for aches and pains, and the Benadryl® makes them drowsy, which helps them sleep. Unfortunately, people who have been taking this for a decade or more have a greater risk of not only liver issues from the Tylenol®, but also a higher risk of dementia because of the diphenhydramine in the Benadryl®.
Save Your Liver, Save Your Life
If you haven’t been to the doctor for a while, it’s very important that you go and get some simple annual tests run. One of them is a Comprehensive Metabolic Panel (CMP). This tests liver function, kidney function, electrolytes and a lot of other things.
But when it comes to your liver, it can tell you if liver enzymes – like ALP, ALT and AST – are going up. And a Gamma-glutamyl Transferase (GGT) Test can measure you GGT levels. When any of these are high, you really have to look into it.
Imaging tests, like an ultrasound, can confirm whether you’ve experienced liver damage or not. And if you’re not an alcoholic, you need to look at other factors. If you don’t take Tylenol®, it has to be from fructose in your diet.
Choose to eat a healthy, fructose-free anti-inflammatory diet. Stay active. Watch your alcohol intake. Look for natural ways to relieve your pain.
And NEVER mix alcohol and Tylenol®.
SOURCES:
Czeisler MÉ, Marynak K, Clarke KE, et al. Delay or Avoidance of Medical Care Because of COVID-19–Related Concerns — United States, June 2020. MMWR Morb Mortal Wkly Rep 2020;69:1250–1257.
Wong RJ, et al. Trends in Liver Disease Etiology Among Adults Awaiting Liver Transplantation in the United States, 2014-2019. JAMA Netw Open. 2020;3(2):e1920294.
Arshad T, Paik JM, Biswas R, Algahtani SA, Henry L, Younossi ZM. Nonalcoholic Fatty Liver Disease Prevalence Trends Among Adolescents and Young Adults in the United States, 2007‐2016. Hepatology Communications. 2021 OCT;5(10).
Adams LA, Lindor KD. Nonalcoholic fatty liver disease. Ann Epidemiol. 2007 Nov;17(11):863-9.
DiNicolantonio JJ, Subramonian AM, O’Keefe JH. Added fructose as a principal driver of non-alcoholic fatty liver disease: a public health crisis. Open Heart. 2017 Oct 30;4(2):e000631.
Kalsi SS, Dargan PI, Waring WS, Wood DM. A review of the evidence concerning hepatic glutathione depletion and susceptibility to hepatotoxicity after paracetamol overdose. Open Access Emerg Med. 2011;3:87-96.
Rotundo L, Pyrsopoulos N. Liver injury induced by paracetamol and challenges associated with intentional and unintentional use. World J Hepatol. 2020;12(4):125-136.
Brune K, Renner B, Tiegs G. Acetaminophen/paracetamol: A history of errors, failures and false decisions. Eur J Pain. 2015 Aug;19(7):953-65.